By Gary Zammit | Forbes Books Author for Forbes Books | AUTHOR POST | Paid Program
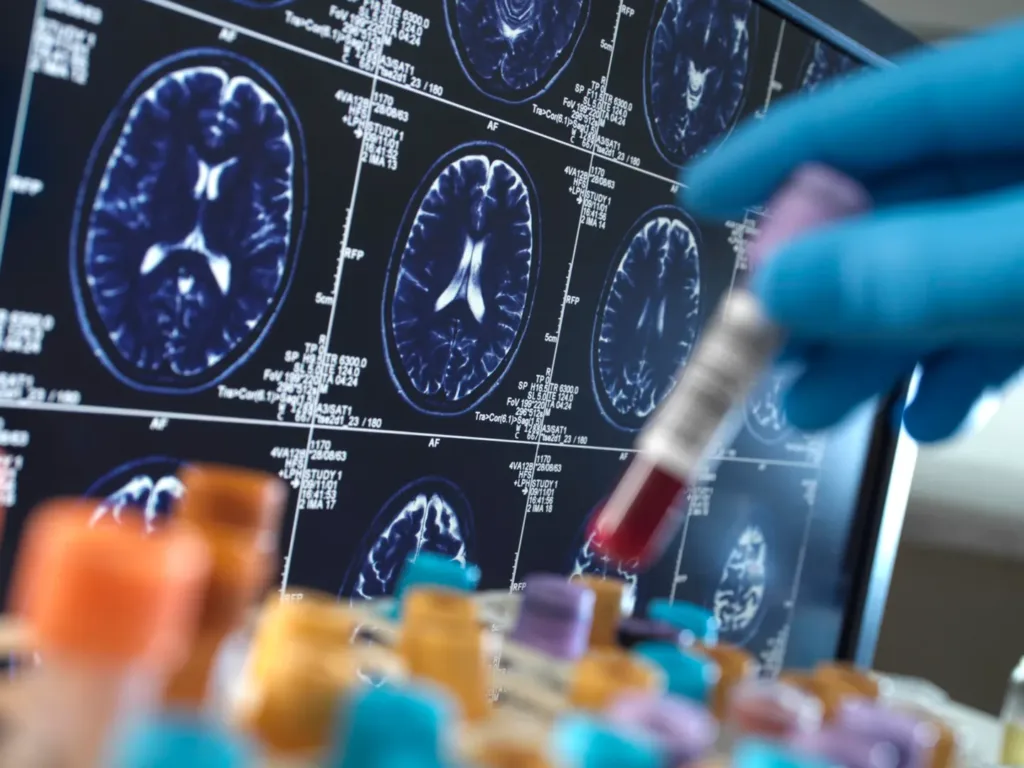
This October saw a landmark development in Alzheimer’s Disease research, with Roche securing clearance from the Food and Drug Administration (FDA) for the first blood-based AD biomarker test. Developed in collaboration with Eli Lilly, the test measures phosphorylated Tau (pTau) 181 protein in human plasma, a key biomarker for Alzheimer’s disease pathology.
This is a significant development, as AD biomarker testing previously required PET scans or invasive spinal taps. In comparison, this simple blood test can be done in regular clinical labs. Approximately 4,500 instruments in clinical labs across the United States can handle the test, making it ready for immediate deployment. For the 92% of patients with mild cognitive impairments who go undiagnosed, this is a promising prospect.
While this is great news, much work remains to be done in AD research. As of now, some 98% of AD drugs fail in Phase II or III clinical trials. Furthermore, many clinical trials focus on identifying biomarker effects rather than considering the patient’s experience. Can we identify patients earlier with blood tests like Elecsys pTau181 and design trials around what matters most to them? Doing so will require returning to the original reason for clinical development: improving patients’ lives.
Identifying the Gap in Alzheimer’s Clinical Trials
Looking at the history of clinical trials in AD, there is a clear gap between what sponsors celebrate and what patients need. While a sponsor might hail the reduction of amyloid plaques (abnormal protein deposits believed to be a hallmark of Alzheimer’s pathology) as a success story, that doesn’t necessarily mean a positive impact for the patient. The patient is more interested in questions like, “Can I still drive my car? Will I recognize my grandchildren?”
We’ve seen the impact of this gap in more than one case, as highlighted in a 2022 paper on clinical trial failures in AD:
- Multiple BACE inhibitors (enzymes that help produce amyloid beta protein—blocking BACE should reduce amyloid formation) have hit targets but worsened outcomes;
- Lanabecestat, a BACE inhibitor, reduced amyloid but showed no clinical improvement;
- Bapineuzumab, a monoclonal antibody designed to clear amyloid plaques, cleared plaques on PET scans but failed to help cognition.
The same paper on failures in AD clinical trials notes that 64% of Phase II and III trials used the Alzheimer’s Disease Assessment Scale-Cognitive subscale (ADAS-Cog) as their primary endpoint. This cognitive test, which has been used for decades, has been shown to have significant limitations for early-stage patients. Essentially, the test is too easy for patients with milder symptoms, resulting in delayed diagnosis. While ADAS-Cog might measure incremental cognitive changes, it fails to capture what matters most to patients, such as instrumental activities of daily living (IADL) and quality of life.
Rethinking Alzheimer’s Disease Research with Patient-Centered Trials
Blood-based biomarkers like Roche’s pTau181 test offer a powerful tool to identify the right patients early, which can enable not only more accurate diagnosis but also broader, more diverse enrollment in trials. Still, identifying patients is only the first step. Moving forward, clinical trial sponsors must focus on the aspects that truly matter to patients and their families, including functional independence, quality of life, and caregiver burden. Drug development protocols must be designed with this principle in mind, prioritizing clinical benefit.
Recent data from Lecanemab trials demonstrate this approach in action. Patients with low tau pathology at baseline (identified through biomarker screening) showed stabilization or even modest improvement in cognitive function. This represents meaningful progress that could potentially translate to patients maintaining their independence for longer.
With Populations Aging, the Time to Act Is Now
More than 55 million people globally have dementia, and most of them have AD. With populations aging worldwide, these numbers are expected to increase, making the need to rethink how we approach Alzheimer’s Disease research imperative. Accessible blood tests like Roche’s promise to help identify patients early. Now, trials must deliver treatments that will actually help them.
Editorial Standards | Reprints & Permissions

By Gary Zammit, AUTHOR POST | Paid Program | Gary Zammit, PhD, founded Clinilabs in 2000, driven by his vision to improve central nervous system drug and device development through specialized contract research. Now an award-winning entrepreneur, he is widely recognized for his expertise in both neuropsychiatric drug development and sleep medicine. As president and CEO of Clinilabs, Zammit leads a team dedicated to advancing treatments for conditions affecting the central nervous system. He simultaneously serves as a clinical professor of Psychiatry at the Icahn School of Medicine at Mount Sinai in New York and is a distinguished Fellow of the American Academy of Sleep Medicine.
Zammit earned his PhD from the University of Toledo, where his work in biological psychiatry earned him both the Turin Service Award and the Leckie Scholar Award. His postgraduate training included an internship and clinical research fellowship at the New York Hospital-Cornell University Medical College, where he was recognized with the Alumni Award for Excellence. Throughout his career, Zammit has authored two books and over 250 articles and abstracts related to clinical practice, sleep, and CNS drug development. His professional mission remains steadfast: developing innovative drugs and devices to treat psychiatric and neurological disorders, ensuring patients have access to better, more effective, and safer treatments that improve health outcomes and quality of life.
Read More: Find Gary Zammit on LinkedIn. Visit Gary’s website. Browse additional work.
